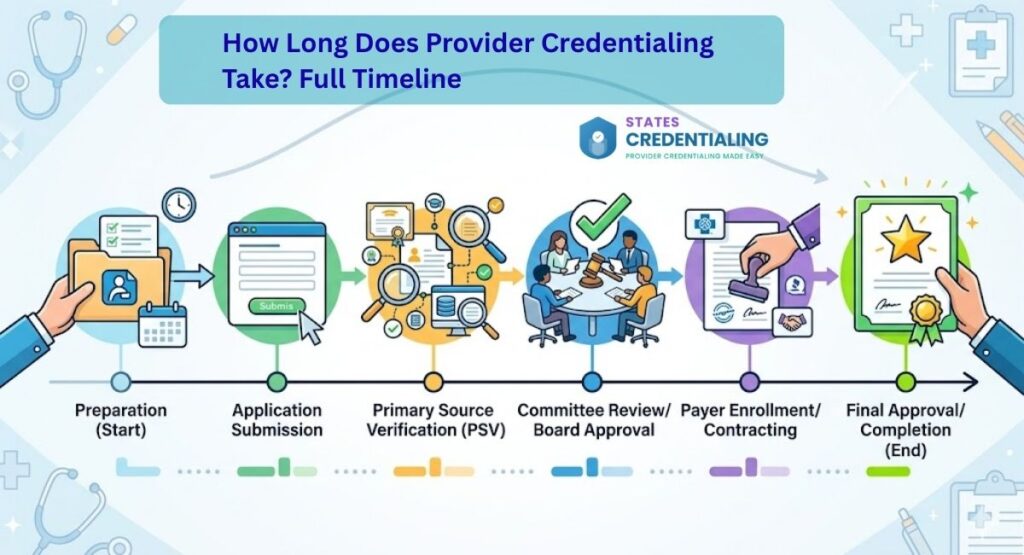
Provider credentialing is one of the first administrative processes that healthcare professionals face when joining a practice, starting a clinic, or working with new insurance networks. Physicians, nurse practitioners, therapists, and other healthcare providers often ask the same question before beginning their payer enrollment journey: how long does provider credentialing take?
The answer is not simple because credentialing involves several verification steps, regulatory checks, and approvals from different organizations. Insurance companies, hospitals, and credentialing databases review a provider’s education, training, licensing, malpractice history, and professional background before allowing them to bill for services.
The credentialing timeline affects many parts of healthcare operations. It influences when providers can begin seeing insured patients, how quickly practices can generate revenue, and whether claims will be accepted by payers. Delays in credentialing can result in lost revenue, postponed patient appointments, and administrative challenges.
For organizations that want to simplify the process, working with specialized teams such as professional provider credentialing services can help manage applications, follow-ups, and documentation requirements while reducing delays.
In this guide, you will learn the complete timeline of credentialing, the factors that influence approval speed, and practical steps to prepare for the process. The goal is to provide a clear manual that explains what happens at each stage so healthcare providers understand what to expect.
Understanding the Purpose of Provider Credentialing
Credentialing is the process used by healthcare organizations and insurance companies to verify a provider’s qualifications. This verification confirms that the provider meets professional standards and regulatory requirements.
The process exists to protect patients and maintain trust in healthcare systems. Insurance companies want to ensure that providers who submit claims are properly licensed, trained, and authorized to deliver medical services.
Credentialing generally includes verification of:
- Medical school education and professional training
- State licensure status
- Board certifications and specialty training
- National Provider Identifier (NPI) details
- Work history and hospital affiliations
- Malpractice insurance coverage
- Sanctions or disciplinary actions
- DEA registration if applicable
Each payer uses credentialing to decide whether a provider can participate in their network and bill for services.
Without credentialing approval, providers cannot receive reimbursement from most insurance companies.
Why Credentialing Timelines Matter for Healthcare Practices
Credentialing timelines influence both clinical operations and revenue management. When providers are not credentialed with insurance networks, claims cannot be submitted or paid.
Some practices allow providers to see patients before credentialing is complete, but reimbursement may not occur until approval is finalized. In other cases, providers must wait until credentialing is finished before seeing insured patients.
Long credentialing timelines can create financial pressure on new practices or expanding clinics. This is why many healthcare administrators research how long does provider credentialing take before hiring new providers or launching services.
Credentialing delays may affect:
- Practice revenue during onboarding periods
- Scheduling for new physicians or therapists
- Patient access to specialized services
- Insurance claim approvals
- Compliance with healthcare regulations
Because of these operational impacts, credentialing planning often begins several months before a provider’s start date.
Typical Timeline for Provider Credentialing
The average credentialing timeline ranges from 60 to 120 days, although some cases may extend beyond this range. Different payers have their own review procedures and verification systems, which explains the variation.
Below is a simplified overview of the standard credentialing timeline.
| Credentialing Phase | Typical Duration | Description |
| Provider Data Collection | 1 to 2 weeks | Gathering personal, educational, and licensing documents |
| Application Submission | 1 week | Sending applications to payers and credentialing databases |
| Primary Source Verification | 2 to 6 weeks | Verifying credentials with schools, licensing boards, and organizations |
| Payer Review and Committee Approval | 3 to 8 weeks | Insurance company credentialing committees review applications |
| Contracting and Enrollment | 2 to 4 weeks | Final contract approval and provider enrollment in payer network |
The timeline above represents an ideal scenario. In reality, missing documents, incomplete applications, and payer backlogs can extend the process.
Step by Step Timeline of the Credentialing Process
To understand how long provider credentialing takes, it is helpful to examine each step individually.
Step 1: Provider Information Collection
The process begins with collecting provider information. Healthcare practices must gather all required documents before submitting applications.
Common documentation includes:
- Medical license copies
- DEA registration
- Board certification documents
- Malpractice insurance certificate
- Curriculum vitae
- Work history verification
- Government identification
- NPI confirmation
Incomplete documentation is one of the main reasons credentialing timelines extend beyond expectations.
Step 2: CAQH Profile Setup
Many insurance companies use the CAQH ProView system to store provider data. Providers must create and maintain an updated profile before payer credentialing can proceed.
CAQH allows insurance companies to access provider information directly rather than requesting documents separately.
Organizations that assist providers with payer enrollment often handle this process through CAQH credentialing support to ensure that profiles remain accurate and up to date.
Providers must also authorize insurance companies to view their CAQH data before applications can move forward.
Step 3: Payer Application Submission
Once documents are ready and CAQH data is complete, credentialing teams submit applications to each insurance company.
Applications may include:
- Payer specific enrollment forms
- CAQH authorization requests
- Tax identification details
- Practice location information
- Billing provider information
Each payer has unique requirements, which means multiple applications may be necessary.
Step 4: Primary Source Verification
After receiving an application, the payer begins verifying provider information with primary sources.
Primary source verification means confirming credentials directly with the organizations that issued them. For example:
- State medical boards confirm licensure status
- Medical schools verify education
- Hospitals confirm privileges and affiliations
- Certification boards verify specialty credentials
This verification process can take several weeks depending on response times from these institutions.
Step 5: Credentialing Committee Review
Once verification is complete, the payer’s credentialing committee reviews the application.
These committees typically meet monthly. If a provider’s application misses a committee deadline, the approval process may be delayed until the next meeting.
Committee review includes:
- Evaluating professional background
- Reviewing malpractice history
- Confirming compliance with network requirements
- Approving or rejecting participation in the network
Step 6: Contract Negotiation and Approval
After committee approval, the payer sends a participation agreement.
The contract outlines:
- Reimbursement rates
- Billing procedures
- Compliance responsibilities
- Network participation terms
Providers must review and sign the agreement before the payer finalizes enrollment.
Step 7: Provider Enrollment and Network Activation
The final stage involves adding the provider to the payer’s system so claims can be processed.
At this stage:
- Provider directories are updated
- Billing permissions are activated
- Network participation becomes effective
After activation, providers can submit claims and receive reimbursements for services.
Average Credentialing Timeline by Payer Type
Credentialing timelines vary depending on the payer category. Government programs often require longer processing periods than private insurers.
The table below shows approximate timelines.
| Payer Type | Average Credentialing Time |
| Commercial Insurance Plans | 60 to 90 days |
| Medicaid Programs | 90 to 120 days |
| Medicare Enrollment | 60 to 120 days |
| Hospital Privileging | 90 to 150 days |
| Managed Care Organizations | 60 to 120 days |
Practices that plan ahead for these timelines can prevent revenue interruptions when onboarding providers.
Factors That Affect Credentialing Timelines
Although average timelines exist, several factors influence how long provider credentialing takes in practice.
Application Accuracy
Incomplete or inaccurate applications are the most common cause of delays.
Missing documents, incorrect license numbers, or incomplete work histories require corrections before review continues.
Payer Processing Volume
Insurance companies often process thousands of credentialing applications each year. When submission volumes increase, processing times may extend.
Primary Source Verification Delays
Credentialing teams rely on external organizations for verification. Slow responses from licensing boards, universities, or hospitals can delay the process.
Provider Work History Complexity
Providers with multiple past employers or hospital affiliations may require additional verification steps.
State Regulations
Each state has its own credentialing regulations and payer requirements. Some states require additional background checks or verification procedures.
Hospital Privileging Requirements
If a provider requires hospital privileges, credentialing may take longer due to additional committee reviews.
Organizations that offer services such as insurance credentialing and payer enrollment support often manage these variables by coordinating communication with payers and verification agencies.
Common Delays in Provider Credentialing
Credentialing delays occur more frequently than many providers expect. Understanding the causes can help healthcare practices prepare.
Common delay reasons include:
- Missing CAQH attestations
- Expired malpractice insurance certificates
- Unverified work history gaps
- Pending state license renewals
- Incomplete payer enrollment forms
- Incorrect practice address information
- Credentialing committee scheduling delays
Another major issue occurs when providers fail to track payer responses after submission.
Regular follow up with insurance companies helps prevent applications from remaining inactive.
Healthcare practices also benefit from learning common mistakes discussed in educational resources such as
Top 4 Mistakes to Avoid During Medical Credentialing
These insights explain why credentialing errors often lead to significant delays in provider onboarding.
Credentialing Timeline for New Practices
New healthcare practices face additional credentialing challenges because they must enroll both providers and the organization itself.
Practice credentialing may include:
- Group NPI registration
- Tax identification verification
- Business structure documentation
- Practice location verification
- Insurance network contracting
Because both the organization and providers must be approved, credentialing timelines can extend beyond standard ranges.
The table below illustrates a possible timeline for new practices.
| Process Stage | Estimated Time |
| Practice registration and NPI setup | 2 to 3 weeks |
| Provider credentialing submission | 2 weeks |
| Insurance verification and review | 6 to 8 weeks |
| Contract negotiations | 2 to 4 weeks |
| Final enrollment activation | 2 weeks |
Planning these steps early allows practices to begin accepting insurance payments sooner.
How Credentialing Affects Healthcare Revenue
Credentialing timelines directly influence practice revenue.
If providers are not credentialed with payers, claims submitted during that time may be denied or delayed.
Revenue cycle experts often highlight how credentialing delays affect financial performance. A helpful discussion appears in
How Physician Credentialing Delays Affect Practice Revenue
The article explains how postponed payer approvals can create revenue gaps during provider onboarding periods.
Healthcare administrators therefore treat credentialing as a key part of revenue cycle planning.
Recredentialing and Ongoing Provider Verification
Credentialing does not end after the first approval. Most insurance companies require recredentialing every two to three years.
Recredentialing ensures that providers maintain professional standards and continue meeting network requirements.
The recredentialing process typically involves:
- Updating CAQH profiles
- Verifying licenses and certifications
- Confirming malpractice insurance coverage
- Reviewing provider performance records
Organizations that handle ongoing provider verification often provide recredentialing services for healthcare practices to track renewal dates and maintain compliance.
Maintaining updated records prevents credentialing lapses that could interrupt billing privileges.
Best Practices to Reduce Credentialing Delays
Healthcare practices can take several steps to shorten the credentialing timeline.
Prepare Documentation Early
Collect provider documents well before the application submission date. Ensure licenses, certifications, and insurance policies remain current.
Maintain Accurate CAQH Profiles
Regularly review CAQH profiles to ensure information remains accurate. Updates should occur whenever licenses, addresses, or employment status change.
Submit Applications Early
Practices should begin credentialing at least 90 to 120 days before a provider’s start date.
Track Application Status
Credentialing teams should follow up regularly with payers to check application status and respond to additional requests.
Use Experienced Credentialing Specialists
Many healthcare organizations rely on credentialing professionals to handle payer communications, document verification, and application tracking.
Professional credentialing teams help maintain compliance while reducing administrative workload for healthcare staff.
Estimated Credentialing Timeline by Provider Specialty
Credentialing timelines may vary by specialty because certain fields require additional verification or payer approval steps.
| Specialty | Average Credentialing Time |
| Internal Medicine | 60 to 90 days |
| Mental Health Providers | 90 to 120 days |
| Cardiology | 90 to 120 days |
| Surgery Specialties | 90 to 150 days |
| Therapy and Rehabilitation | 60 to 90 days |
These timelines depend on payer requirements and credentialing committee schedules.
Credentialing Checklist for Healthcare Providers
Before starting credentialing applications, providers should confirm that they have the following documents ready.
Credentialing preparation checklist:
- Current state medical license
- DEA registration if applicable
- Board certification documents
- Curriculum vitae with full work history
- Malpractice insurance certificate
- National Provider Identifier confirmation
- Government issued identification
- Hospital privilege documentation if required
Maintaining a digital file with these documents simplifies credentialing submissions for multiple insurance networks.
Technology and Credentialing Efficiency
Modern healthcare organizations increasingly use credentialing software and automated systems to manage provider data.
Digital credentialing platforms help track application status, manage documents, and communicate with payers more efficiently.
Technology also improves coordination with revenue cycle management systems and insurance verification processes. Discussions on healthcare billing integration appear in resources such as
Leading EHR / EMR Systems Integration with Medical Billing
Efficient technology systems reduce administrative workload and help credentialing teams monitor deadlines and payer responses.
Credentialing and Hospital Privileging
Hospital privileging is a related process that allows providers to treat patients within hospital facilities.
Although credentialing verifies qualifications, privileging determines what procedures providers may perform in the hospital.
Hospital privileging may include:
- Clinical competency evaluation
- Department committee review
- Peer recommendations
- Procedure authorization review
Hospitals typically conduct these evaluations through dedicated committees that meet periodically, which can extend approval timelines.
Manual Guide Summary: Credentialing Timeline Overview
The table below summarizes the entire credentialing timeline for quick reference.
| Stage | Main Tasks | Estimated Duration |
| Document Preparation | Collect provider credentials and records | 1 to 2 weeks |
| CAQH Profile Setup | Create or update CAQH profile | 1 week |
| Application Submission | Send enrollment forms to payers | 1 week |
| Primary Source Verification | Verify licenses, education, certifications | 2 to 6 weeks |
| Committee Review | Payer credentialing committee approval | 3 to 8 weeks |
| Contracting | Review and sign participation agreements | 2 to 4 weeks |
| Network Activation | Provider added to payer system | 1 to 2 weeks |
In most situations, the entire process ranges from two to four months.
However, complex cases or high application volumes may extend the timeline further.
Final Thoughts
Understanding how long does provider credentialing take helps healthcare providers and administrators plan for successful practice operations. Credentialing is a detailed verification process designed to maintain patient safety and ensure that healthcare professionals meet industry standards.
The complete timeline includes document preparation, application submission, primary source verification, payer review, and contract approval. Each stage requires careful coordination between providers, insurance companies, licensing boards, and credentialing committees.
Healthcare organizations that prepare documentation early, maintain updated CAQH profiles, and track payer responses can reduce delays and improve the efficiency of credentialing approvals.
For practices seeking structured guidance and administrative support, professional teams such as States Credentialing assist with the entire process from documentation management to payer enrollment. Their services help healthcare providers navigate credentialing requirements while maintaining compliance with insurance networks and regulatory standards.
Helpful Resources
The following resources provide additional information about credentialing, billing, and healthcare revenue management:
- Provider Credentialing Guide
- Streamline Your Provider Credentialing Process
- Insurance Payer Credentialing Guide
- CAQH Credentialing for Mental Health Providers
These resources expand on credentialing processes, payer enrollment strategies, and administrative best practices for healthcare providers.